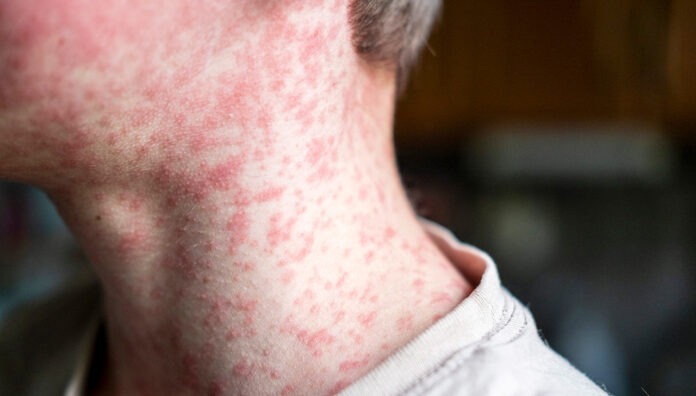
From the United States to Europe, India and Southeast Asia – measles cases have been exploding worldwide.
In Texas, a measles outbreak with more than 500 cases is ravaging the state – leading to the death of an unvaccinated 6-year-old child. In our own backyard, an outbreak is fast developing in Western Australia – with 10 confirmed cases, and counting. Almost 40 measles cases have been confirmed across Australia this year.
The measles mumps rubella (MMR) vaccination rate in Texas among kindergarten-aged children is 94.3% – slightly below the World Health Organization’s 95% target.
Australia’s vaccination rate for all 5-year-olds is lower, sitting at 93.76%

So are we headed for Texas territory? Australian Pharmacist sat down with Professor Margie Danchin, group leader of the Murdoch Children’s Research Institute’s (MCRI) Vaccine Uptake Group, to find out.
Is Australia at risk of losing control over measles spread?
To really stop measles transmission, a herd immunity threshold between 93–95% coverage is required. But many areas of the country are well below this figure.
This includes the Noosa Hinterland and the Northern Rivers region of New South Wales – where coverage (two doses of the MMR vaccine) only sits between 70–75%, said Prof Danchin.
‘Measles can spread pretty quickly in a low-coverage population,’ she said. ‘There will be local transmission from secondary cases because there just isn’t that coverage there to stop it spreading.’
In a population with 70–75% overage, one case could infect approximately 5–8 people, and then each one of those people can infect another 5–8 people. ‘In low-coverage areas, cases need to be quickly isolated to stop transmission occurring, otherwise it can take off like a wildfire – which is exactly what’s happened in the US.’
What’s driving the surge in measles cases?
A range of factors, Prof Danchin said. Take the current outbreak in Texas for example.
‘Geopolitics and the views of the current administration about vaccines being a personal choice is having some impact already,’ she said. ‘But it wouldn’t be the whole story.’
Since the COVID-19 pandemic, vaccine coverage rates for children have decreased globally due to a complex mix of access and acceptance factors – leaving gaps in coverage that can fuel an outbreak.
In Australia, access barriers are the key driver for partially vaccinated children under 5 years, as identified by the MCRI, University of Sydney and National Centre for Immunisation Research and Surveillance’s (NCIRS) Vaccination Insights Project.
‘We measured nationally the main drivers of low vaccine coverage in Australia among partially and totally un-vaccinated children,’ Prof Danchin said.
‘And the strongest drivers for partially vaccinated kids were practical barriers – including not being able to get an appointment with the GP, or not being able to afford the costs associated with vaccination.’
Because many GPs don’t bulk bill anymore, parents are forced to pay gap payments, along with taking time off work, needing to find childcare for other children and possibly transport costs.
‘It’s usually practice nurses who administer the vaccines in general practice, and they might not work full time, or only work once a week,’ she said.
In regions such as the Northern Rivers, hesitancy is likely the driving factor, Prof Danchin said.
‘There’s a lot more mistrust in vaccines, providers and institutions post-COVID-19. Because the vaccines were under such intense scrutiny, vaccine safety concerns were really amplified in the media,’ she said.
‘At least 10% of the population still have a concern that the MMR vaccine can cause autism, despite 25 years of research that conclusively disproves the link.’
How can pharmacists promote the importance of vaccination?
By clearly communicating the benefits of vaccines while acknowledging the risks of vaccine-related adverse events.
‘We’ve got to be careful that we don’t oversell vaccine safety,’ Prof Danchin said. ‘We need to be clear that tall vaccines have common and expected side effects, and that serious side effects are very rare.’
Given MMR is a live vaccine, patients can expect side effects around 1 week after receiving the vaccine. This can include a fever, coryza and a rash
But the key is communicating the risk-benefit to patients. ‘One in five people who get measles will have to go to hospital, one in 20 will get pneumonia and one in 1,000 will get inflammation of the brain or encephalitis – so the risks associated with contracting measles are high, especially among the most vulnerable such as babies under 1 year or children who have lowered immune systems,’ she said. ‘It is our responsibility to protect everyone in the community, especially those who cant be vaccinated with live vaccines.’
A communication strategy based on respect, listening and motivational interviewing can also help pharmacists understand where a person sits on the vaccine hesitancy spectrum.
‘For example, we need to assess if the parent is a true refuser or are they a bit of a fence sitter?’ Prof Danchin said. ‘Do they just want to partially vaccinate or do they want to vaccinate fully, but just have some questions?’
The next step is to listen to their concerns and validate them, then ask permission to share information and point them to trustworthy sources.
‘If they’re not ready, invite them to come back,’ she said. ‘It’s not coercive and should bring people down from that heightened space of wanting to argue or defend themselves to genuinely being more receptive to the information.’
Pharmacists cal also refer to this resource, developed by a team of researchers and clinicians for parents and providers to help everyone have more non-judgmental conversations.
Who is eligible for a catch-up dose?
Anyone who is partially vaccinated. This also includes adults who were born between 1966 and 1992, with the two-dose schedule of the MMR vaccine only being introduced in Australia in 1992.
If patients are unsure about their or their children’s vaccination status, pharmacists can check the Australian Immunisation Register or advise patients to do so.
Different jurisdictions allow pharmacists to administer the MMR vaccine to children of various ages, so pharmacists should check the regulation in their state or territory before offering a catch-up vaccination.
Patients can receive a funded MMR vaccine under the NIP until 19 years of age, Prof Danchin said.
‘We recommend they get a second dose, because one dose of the MMR vaccine only provides about 91–93% protection,’ Prof Danchin said.
‘While people who’ve had one dose are more likely to get less severe measles, they can still get quite sick.’
How important is vaccination prior to travel?
Ahead of the Easter holiday break, NSW Minister for Health Ryan Park has called on people planning to travel overseas this April to ensure they and their family are fully protected against measles, with large outbreaks currently in many countries including Vietnam and other parts of Southeast Asia.
‘Measles is one of the most infectious diseases there is, and we are concerned about it spreading quickly in under-vaccinated communities,’ he said. ‘Anyone who is not immune is at risk of developing the disease if they are exposed.’
It’s particularly pertinent that both adults and children who are planning to travel are up to date with their two MMR vaccine doses.
‘Pharmacists should ask, “Are your kids up to date? Are you up to date?” And highlight the fact that you can get a catch-up dose, as one dose doesn’t give you high enough protection,’ Prof Danchin said.
Pharmacists can advise parents that children under the eligible vaccination age can also receive protection prior to travelling.
‘Infants aged 6–11 months can be offered a free additional dose of the MMR vaccine in Victoria and NSW so they have at least some protection from measles if they’re traveling through airports and on planes,’ she said. ‘But they still have to get their 12 and 18 month doses.’
Those who can’t get vaccinated, such as pregnant people or patients who are immunocompromised, can receive human immunoglobulin up to 6 days after an exposure.
‘And those who are not up to date with their MMR vaccine can get a dose within 4 days of an exposure,’ Prof Danchin added.


 Dr Peter Tenni[/caption]
Dr Peter Tenni[/caption]
 How should we deprescribe gabapentinoids, according to the Maudsley Deprescribing Guidelines[/caption]
How should we deprescribe gabapentinoids, according to the Maudsley Deprescribing Guidelines[/caption]



 Pharmacists have always prescribed, but they have the potential to prescribe much more
Pharmacists have always prescribed, but they have the potential to prescribe much more