Over the weekend, the Albanese Government announced a $573 million commitment to national women’s health initiatives, to bipartisan support.
So what is actually happening? And when?
Australian Pharmacist takes a ‘deep dive’ to help pharmacists navigate these life-changing initiatives for women.
Two new oral contraceptive pills listed on the PBS
What: oral contraceptive pills (OCP) Yaz (drospirenone/
When: From 1 March 2025
Why: the Pharmaceutical Benefits Advisory Committee (PBAC) recommended adding Yaz and Yasmin to the PBS with no restrictions applied to the therapeutic use – noting women’s preference for having more subsidised combined oral contraceptive (COC) pill options to choose from.
However, there is insufficient evidence to demonstrate Yaz or Yasmin offer clinical advantages over existing PBS-listed COCs, including lowering fluid retention, blood pressure, and acne management – despite public perception.
And the adverse effects, in fact, could be worse, including a heightened risk of venous thromboembolism.
Impact: up to 50,000 women are expected to benefit from the decreased cost of drospirenone with ethinylestradiol, with costs set to drop from $380 per year to $126.40, or $30.80 with a concession card.
‘Yaz and Yasmin are both commonly used combined oral contraceptives, with a range of indications to support women’s reproductive healthcare,’ said PSA National President Associate Professor Fei Sim FPS.

‘Patients who meet the eligibility criteria will be able to access these medicines at a PBS-subsidised price, making access more affordable and equitable.’
Three new MHTs also set to be included on the PBS
What: the menopausal hormone therapies (MHTs) Estrogel (estradiol), Prometrium (progesterone) and Estrogel Pro (estragio/progesterone) will also be listed on the PBS – marking the first MHT listings in 20 years.
When: from 1 March 2025
Why: various MHTs, including strengths of Estalis (estradiol /norethisterone acetate) and Estradot (estradiol) transdermal patches, have been in short supply for months, forcing women to pay hundreds of dollars annually for substitutions under Section 19A of the Therapeutic Goods Act or newer, unsubsidised MHTs.
The TGA has also warned that supply shortages of some PBS-listed menopause treatments will persist throughout 2025.
PBAC recommended the listing of Prometrium, Estrogel and Estrogel Pro as General Schedule unrestricted benefit listings, with corresponding General Schedule restricted benefit listings for 60-day maximum dispensed quantities.
These new PBS subsidies also follow a 2024 Parliamentary Inquiry recommendation to make newer menopause therapies more affordable and accessible.
And because these medications match the body’s own hormones more closely, many women find they experience fewer or milder side effects compared to older therapies.
Impact: the new PBS subsidies mean women will soon be able to pay substantially less for modern menopause therapy – reducing the cost from around $650 per year to as little as $7.70 or $31.60 a month for around 150,000 women.
‘Prometrium, Estrogel and Estrogel Pro are all commonly used hormone replacement therapy,’ said PSA National President Associate Professor Fei Sim FPS.
‘Having them on the PBS means they will be subsidised for women who need them, better supporting women experiencing perimenopause and menopause.’
A national approach for OCP access and treating uncomplicated UTIs directly from pharmacies
What: national OCP and urinary tract infection (UTI) pharmacy trials, allowing pharmacists to initiate PBS medicines for the first time ever.
When: early 2026. At this stage, these trials are part of Labor’s election platform, however the coalition has vowed to match this measure.
Why: the nation-wide trials are designed to boost access to treatment for uncomplicated UTIs and hormonal contraception through community pharmacists at PBS medicine cost.
Impact: around 250,000 concession cardholders will be able to consult a trained pharmacist free of charge. And if medication is required, they will only need to pay the standard cost of the medicine.
Enabling appropriately trained pharmacists to prescribe treatment for uncomplicated UTI and contraceptives under the PBS will allow for equitable, affordable healthcare for women and girls, said A/Prof Sim.
‘We all know that when experiencing symptoms of UTI, timely treatment is critical,’ she said.
Previously, when prescribing and management of these acute conditions were undertaken, patients often faced additional out-of-pocket costs to see a pharmacist versus a GP.
‘[Allowing] pharmacists to prescribe treatment under the PBS means there is no discrimination with care,’ she added.
Widened access to long-term contraceptives at a lower cost
When: unknown at this stage. The coalition has vowed to match this measure.
Why: only 6% of Australian women use an Intrauterine device (IUD), with 5% opting for the contraceptive implant – partly due to a lack of awareness about these options.
Access is further impacted by difficulties finding trained GPs, coupled with long waiting times, for insertions.
While a slight Medicare rebate increase was introduced in 2022, it doesn’t cover the costs and time required for IUD insertion – discouraging many GPs from offering the service. The high cost of training also makes it challenging for GPs to gain the necessary qualifications.
Impact: the new women’s health package improves access to IUDs and implants by increasing clinician rebates and introducing Medicare coverage for nurse practitioner insertions. It also incentivises GPs to bulk bill insertions, eliminating out-of-pocket costs for women. Eight training centers will also be established across Australia to enhance clinician skills and confidence in IUD insertion.
‘This should make it more affordable and much easier for women to find a clinician to insert it,’ said Danielle Mazza, Director, SPHERE NHMRC Centre of Research Excellence in Women’s Sexual and Reproductive Health in Primary Care.
New Medicare support for menopause
What: a new Medicare rebate for menopause health assessments
When: from 1 July 2025
It is unclear when funding to train health professionals, a first-ever clinical guideline for menopause and a national awareness campaign will be introduced. But the coalition has vowed to follow through with these initiatives if reelected.
Why: as one caller to 774 ABC Radio Melbourne put it this week, ‘women are just used to putting up with stuff.’
‘I’ve always had the feeling that once you hit 65, once supposedly you’ve had your kids and you’ve helped a bit with the grandchildren that basically medically you’re just forgotten,’ the caller continued.
The menopause initiative should help to shift that narrative, designed to support women experiencing menopause and perimenopause to receive appropriate care from their GP, and help to ensure informed conversations with trained healthcare professionals.
Impact: a 2024 Parliamentary inquiry into menopause found GPs have limited knowledge and perimenopause and menopause and are often unable to recognise symptoms.
Boosting healthcare education and knowledge, along with empowering women to advocate for their own health, should help to address this.
More clinics to address endometriosis and pelvic pain
What: 11 new clinics dedicated to endometriosis and pelvic pain will be opened, along with 33 existing clinics receiving more staff to provide specialist support for menopause
When: an unspecified date after the federal election. The coalition has vowed to match these initiatives if elected.
Why: endometriosis affects around one in 7 Australian women by age 44–49, often leading to severe pelvic pain, fertility issues, irritable bowel syndrome or mental health issues. Yet despite advancements in medicines and surgical treatments, there is still a high rate of recurrence.
A Victorian inquiry into women’s pain and health also found that the pain women experience is often overlooked.
Impact: through more healthcare avenues, women can benefit from improved access to diagnostic, treatment and referral services for endometriosis and pelvic pain.
The announcement will break down barriers to healthcare access, especially in regional, rural and remote areas, reflecting the recommendations and work of the National Women’s Health Council, said A/Prof Sim, who co-chairs the Access, Care and Outcomes Subcommittee.
‘These are the recommendations our Council has been calling for,’ she added.
A summary of these announcements is below:
| What | When | Detail |
| Listing of two additional oral contraceptive pills on the PBS | 1 March 2025 | Yaz and Yasmin will be listed on the PBS as unrestricted benefits |
| Listing of three additional menopausal hormone therapies on PBS | 1 March 2025 | Estrogel, Prometrium and Estrogel Pro will be listed on the PBS as unrestricted benefits |
| Pharmacy trials of OCP prescribing and treating uncomplicated UTIs | Early 2026* | Free-of-charge UTI and OCP consultations in community pharmacies for concession card holders, with prescribed medicines available via the PBS |
| Increased access to long-term contraceptives | Unknown* | Increased rebates and new Medicare rebates for IUD and hormonal implant insertions.
Eight training centres to be established to increase clinician skill and confidence |
| Medicare support for menopause | From 1 July 2025 | New Medicare rebate for menopause health assessments
Training, guidelines and a public awareness campaign will also be developed |
| Additional endometriosis and pelvic pain clinics | Unknown* | 11 new clinics (in addition to 33 currently existing) dedicated to endometriosis and pelvic pain |
* subject to incoming government meeting election commitments
Find out more about supporting women through menopause by attending the ‘Mastering menopause care in pharmacy practice’ session at the NSW Annual Therapeutic Update, held from Friday 28 February to Sunday 1 March 2025. Register here to attend.



 Categorisation of heart failure
Categorisation of heart failure A focus on SGLT2is
A focus on SGLT2is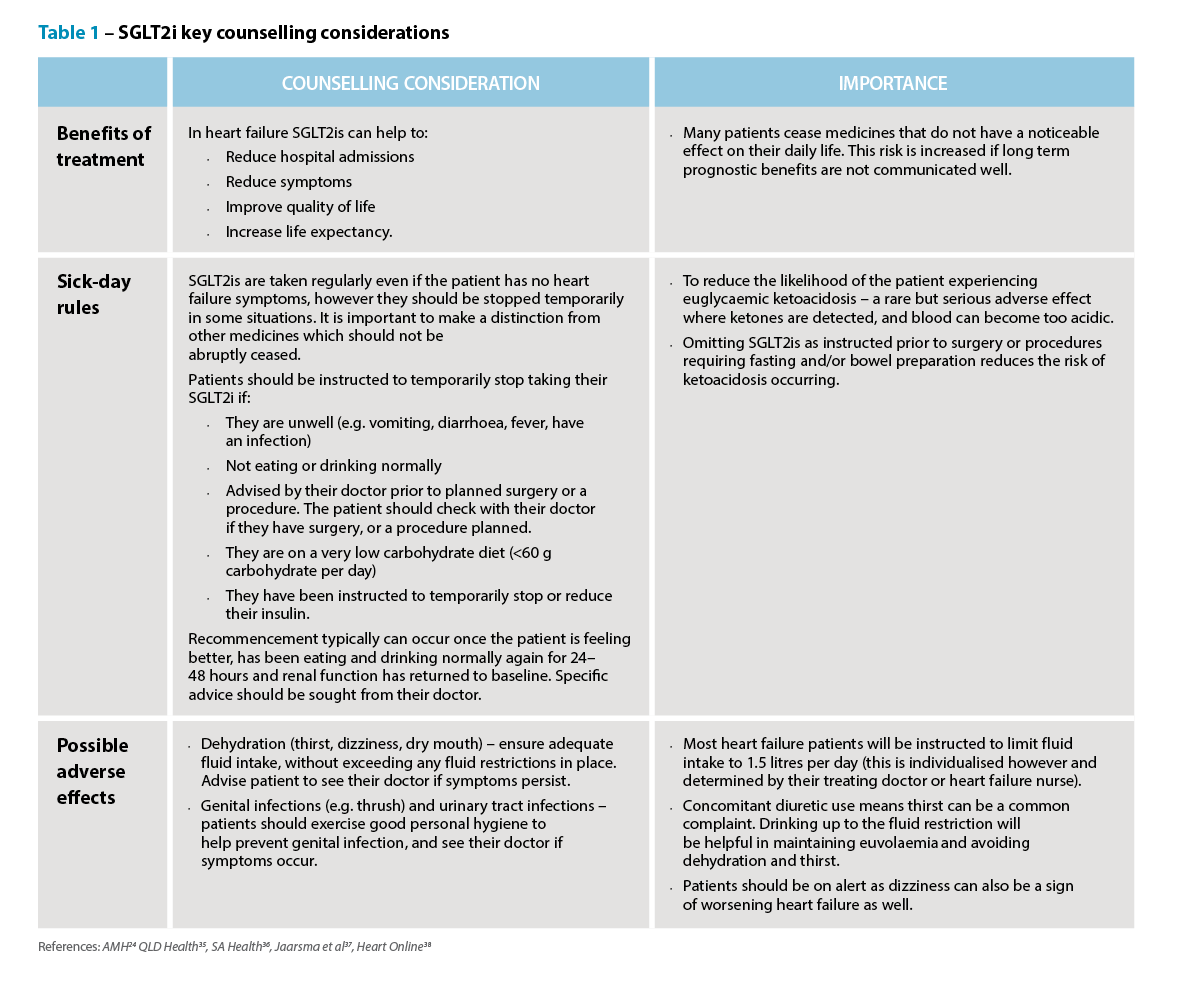 Knowledge to practice
Knowledge to practice 
 Professor Anthony Lawler, Australian Government Chief Medical Officer,
Professor Anthony Lawler, Australian Government Chief Medical Officer, 
 This CPD activity is supported by an unrestricted education grant by Reckitt.[/caption]
This CPD activity is supported by an unrestricted education grant by Reckitt.[/caption]
 Case scenario
Case scenario